Turn Reimbursement Data into a Strategic Advantage in Payor Contracting
Successful payor contracting starts with real data — not estimates or outdated surveys. With Payorology, practices can now access the current reimbursement rates payors have agreed to with their peers in the same community, for every CPT® code, down to the penny.
This level of visibility gives you an edge in payor contract negotiations. With monthly updated data pulled directly from payors, you can see exactly what insurers are reimbursing for every service, across every practice in your market. No more guesswork. No more relying on anecdotal benchmarks.
Whether you’re preparing for payor contracting negotiations, exploring partnerships, or assessing your market position, price transparency healthcare data gives you the clarity to act with confidence. By comparing rates CPT® code by CPT® code, you can identify opportunities, strengthen your negotiating position, and ensure your reimbursement rates are aligned with market reality.
Payorology transforms raw medical price transparency data into clean, actionable insights—so you spend less time decoding data and more time using it to drive smarter payor contracting decisions.
The information asymmetry that costs practices millions
For decades, payor contract negotiations have been structurally imbalanced. The payor's contract team knows exactly what they're paying every other practice in your market for every CPT® code on your fee schedule. The practice across the table has only their own contract history, their general sense of what seems reasonable, and whatever their billing consultant has heard through the industry.
That asymmetry has a dollar value. A practice sitting 30 percent below market rates on its five highest-volume CPT codes — compounding across a three to five year contract term — is leaving a significant amount of revenue on the table. Not because they negotiated badly. Because they negotiated without the information they needed.
Price transparency data has changed the information landscape. For the first time, practices can know — specifically, by code, by payor, by market — what comparable providers are actually being paid. The practices that are using this data in their contract negotiations are consistently achieving better outcomes. The ones that aren't are still negotiating in the dark.
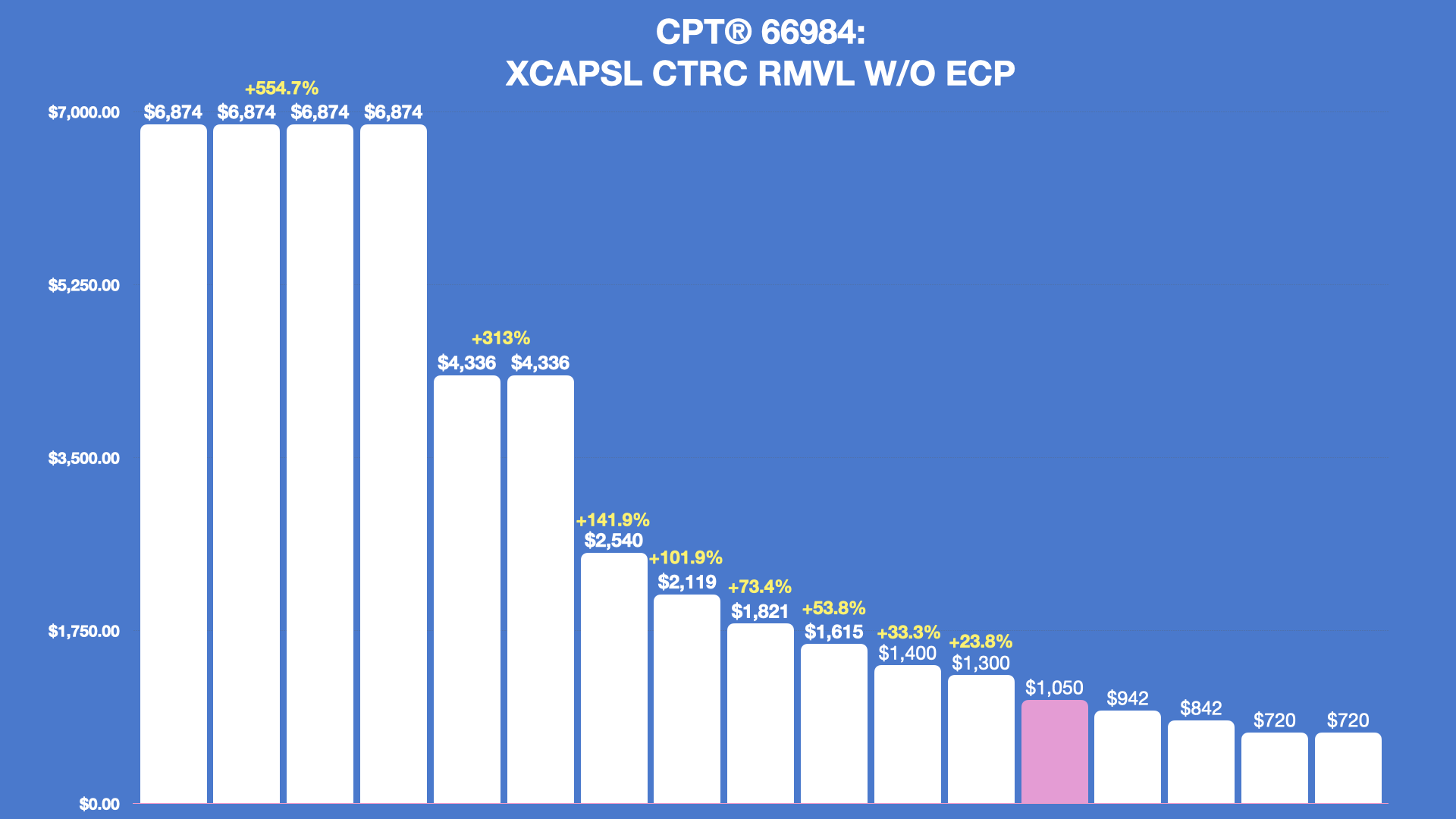
Example Rates
Below is an example of facility rates for Ophthalmology ASCs for CPT® 66984. These are identified as facility rates based on service codes, NPIs, and additional data provided in the files. The differences in payor reimbursements can be dramatic — and understanding them is key to effective payor contracting.
What a data-informed payor contract negotiation looks like
The most effective payor contract negotiations share a common structure. They begin not with a request — 'we want higher rates' — but with a market-grounded case: 'we have reviewed what you are paying comparable practices in this market, and we'd like to align our contract with those rates.' That shift in framing changes the entire conversation.
A payor's contract team can deflect a preference indefinitely. They cannot easily dismiss a specific, documented request tied to their own publicly disclosed rates. The negotiation becomes a discussion about market alignment rather than a negotiation about what the practice deserves.
- Step 1 — Identify your highest-value CPT codes
Start with the procedure codes that represent the largest share of your annual revenue. In most specialty practices, 20 to 30 codes represent 70 to 80 percent of total collections. A focused renegotiation on these codes will have more financial impact than a broad push across the entire fee schedule. - Step 2 — Pull peer rate benchmarks for those codes
Using price transparency data, establish what comparable practices in your market are being reimbursed by the same payor for the same codes. This is your benchmark — not what you ideally want to be paid, but what is already being paid to someone like you, right now, by the same insurer. - Step 3 — Calculate the gap and prioritize
For each code and each payor, calculate the difference between your current rate and the peer benchmark. Rank these gaps by dollar impact on annual revenue. The highest-impact gaps become your negotiation priorities — the specific asks that will move the needle most. - Step 4 — Build a specific, defensible rate request
Your rate ask should cite market evidence, not just practice economics. 'We've seen that comparable practices in this market are being paid X for this code' is a statement the payor has to respond to. It grounds the conversation in their own disclosed data and makes it very difficult to simply dismiss. - Step 5 — Start early
The optimal time to begin preparing for a contract renegotiation is 12 to 18 months before expiration. That window lets you pull the data, analyze it, and approach the payor on your timeline rather than theirs. Payors are accustomed to practices that arrive at the table unprepared and under time pressure. Arriving early and armed with market data is itself a signal that this negotiation will be different.
WHAT WE SEE IN NEGOTIATIONS
Practices that enter a renegotiation with vetted peer rate benchmarks consistently achieve better outcomes than those that don't. The data changes what they ask for — because for the first time they know what to ask for. It also changes how the payor responds. A specific, market-grounded request is much harder to deflect than a general ask for better rates.
The timing and compounding problem
One of the most underappreciated dynamics in payor contracting is how rate gaps compound over time. A practice that accepts a modest annual increase from a below-market starting point doesn't close the gap with a better-positioned competitor — it falls further behind. Both practices are getting annual increases, but the practice at the top of the market distribution is getting them from a higher base.
Over a five-year contract cycle, a practice that was 25 percent below market rates at the start may find itself 30 percent below market by the end — even if it received annual increases each year. The only way to close a structural rate gap is through a deliberate renegotiation that targets the gap specifically, with market evidence to support the ask.
Payor contracting across your portfolio
For PE-backed groups and large multi-state practices, payor contracting is not a practice-by-practice problem — it is a platform-level opportunity. Rate benchmarking across a portfolio reveals which entities are most below market, which renegotiation windows are coming up across all locations, and where a coordinated negotiation strategy could yield the most significant revenue improvement.
The same analysis that prepares a single practice for a contract renewal can be applied across 10, 20, or 50 locations to build a prioritized renegotiation roadmap — sequenced by contract expiration dates and ranked by revenue uplift potential.
HOW PAYOROLOGY WORKS WITH YOU
Payorology is not just a self-serve platform. We build a curated, vetted benchmarking portal for your specific specialty, your specific markets, and your specific payor relationships — and our team works with you to interpret it and translate it into a negotiation strategy. Our clients describe us as their price transparency department: an expert team that happens to sit outside their org chart. When there is a contract on the table, that distinction matters.
Related resources in the Knowledge Center
→ See what comparable practices in your market are being paid. Request a consultation

Have questions? Reach out!
If you think we may be able to help, let's meet for 30 minutes. No pressure, we promise.
This site is protected by reCAPTCHA and the Google Privacy Policy and Terms of Service apply.
